
Healthcare and Generative AI: 7 Ideas for 7 Ages
When we discuss Generative AI (GenAI) with customers, we often find that one of the initial barriers to understanding is that people don’t yet grasp what GenAI is for. Customers will throw out an entire bucket list of ideas, 99% unrelated to GenAI. And that’s understandable; if your organisation is facing existential pressures, you care about solving those problems, rather than tinkering around with the latest gadget to understand how it can help.
With that context in mind, it felt like an interesting thought exercise to see if we could develop a set of practical use cases for GenAI adoption within healthcare. To help frame the exercise, we’ve listed out seven ideas across the ‘seven ages’ of life. These are nothing more than ideas, and some of them might well turn out to be implausible or impractical, but hopefully, you’ll find the process illuminating, and who knows, perhaps it will help you formulate some ideas of your own for your part of the world.
HEALTHCARE PRESSURES
Before we dive into the seven ideas, it’s helpful to refresh our memory of why this is a necessary conversation within healthcare in the UK. The NHS is currently under extraordinary pressure, and with the healthcare industry historically at the forefront of technological innovation, it is no surprise that the use of AI has emerged as a potential saviour. We can break down the current pressures on the NHS into four core areas.
Demand/capacity. The UK population is ever-increasing, and more bodies equals greater demand for the healthcare system. We continue to be in the long tail of COVID, where waiting lists grew due to disruption within the NHS, which in turn puts increased strain on current services. It’s also historically been the case that the NHS has been run “hot”, with minimal spare capacity to maximise efficiency. That’s fine when fluctuations in demand remain relatively static, but not so great when demand surges.
Complexity. The growing population is partly down to people living longer. Longer life means that healthcare demands become more onerous through what the medical profession terms ‘co-morbidities’, i.e. multiple simultaneous health conditions. As well as those co-morbidities, we also find that people are suffering from greater numbers of long-term conditions (e.g. long covid). And with older people, there’s usually additional complexity from cases that fall between multiple organisations (e.g. healthcare from the NHS and social care from a local authority).
Costs. We’ve all been feeling the hit from inflation over the past few years, and the NHS is no different. Costs have risen, and the NHS budget hasn’t kept up. And as much as we might love it, even the most ardent defender of the NHS must admit that there are inefficiencies in the way the system is run.
Staffing. The NHS has, for a long time, not had the levels of staffing it wants at all levels. For example, nursing numbers are 10% down on where they “should” be, and there’s a long-term decline in GP numbers.
Putting this together we have an NHS that’s being asked to deliver more, but with fewer resources. And that’s where GenAI might be able to help plug a few gaps.
SEVEN AGES: BIRTH
The first of our seven ages is birth, and the obvious area to look at is maternity care. There are numerous problems with maternity care in the UK, but one that’s been highlighted by the Nuffield Trust is the disparity in outcomes across demographics:
“Women of Black ethnic backgrounds were four times more likely than white women to die in childbirth… Likewise, women living in the most deprived areas had a maternal mortality rate two-and-a-half times higher than women living in the least deprived areas”
So why is that the case? There are likely to be many reasons, but a few that have been highlighted are:
- Staffing – staffing levels vary widely across the UK’s hospital Trusts, and depending on where you live you may get a different standard of care
- Continuity of care – Ideally you would see the same team through pregnancy and right up to childbirth, but staffing pressures mean that’s not always the case
- Level of personalisation – Quite obviously, pregnancy is an incredibly personal experience, and people must be able to tailor their pregnancy to their own needs. Sometimes some barriers make this harder for certain groups.
So where does GenAI fit? Improving personalisation is one of the NHS’s core stated goals for maternity care, and GenAI could help.

At the heart of the interactions between pregnant mothers and the maternity team is the “care plan”, historically a giant stack of bits of paper and leaflets, with some additional detail on an electronic record. This gets physically carried around and used as the basis for discussions with the midwives. Inside are the decisions and expectations of the pregnant mother. In many areas, this is now being switched to an app-based electronic approach, but even so, there is a lot of information to digest and important decisions to be made and recorded.
If English isn’t your first language, or you’re not the best at reading comprehension, this can be a bit overwhelming. One of GenAI’s strengths is the ability to personalise content. Perhaps with the advent of electronic versions of care plans, they can be re-envisaged as an interactive, living, ongoing conversation with the mother. GenAI could act as a helpful intermediary that ensures everyone understands the decisions that need to be made, is given evidence in a way that makes sense, and ensures that everything is accessible and open.
CHILDHOOD
Next, childhood. Vaccine hesitancy is an increasing problem in the UK.
To maintain herd immunity for diseases such as measles, 95% of children need to be immunised. Current figures put the number at 85%, and in some areas of the country, below 60%.
So why is that? We are all familiar with the vaccine scepticism that emerged during COVID, and was amplified across social media. Vaccine misinformation is nothing new, dating back decades to the MMR scandal. But there are also issues with convenience, and the ability of working parents to find time to get their kids vaccinated. And lastly, there’s a need to deliver messaging around vaccination in different ways to different communities, and the NHS hasn’t always been able to do that.
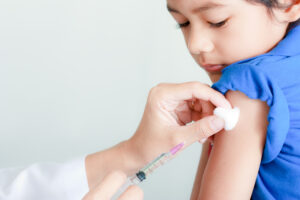
So where does GenAI fit here? Well, social media seems a good place to look. According to the BMJ, medical officials struggle to keep pace with the volume of misinformation online. And that’s not surprising, there’s an army of (misguided) volunteers online ready and waiting to share and re-post misleading information about vaccines, and a comparatively small number of public health professionals leading the charge to get positive messaging out.
GenAI could change all that. GenAI tools are excellent at creating content and adapting it to suit different audiences. Via targeted use of GenAI, the volume and quality of informative vaccine content could be exponentially increased across multiple channels, taking account of differing community needs and effectively getting the positive message across before the social media vaccine sceptics spread misinformation.
ADOLESCENCE
Mental health is an ever-increasing problem in younger people.
According to research, the number of young people reporting mental health problems has increased from 1 in 9 to 1 in 6 over the past few years, with the number of referrals to mental health crisis teams trebling over the same period. Partly this is due to chronic underfunding which means mental health provision has plummeted and waiting lists ballooned. But there are also unique pressures on a demographic that’s growing up immersed in a digital world to a greater extent than any others before.
So how can GenAI help? Well, leaning into the digital aspect of mental health could be an option. It’s already the case that various digital tools are being trialled to help alleviate mental health pressures, and while older demographics might hate the idea of an app to help your mental health, younger generations are already well-versed in living in a digital environment. There are two areas where GenAI might help.

The first is through the provision of tailored apps and games which have been developed to get younger audiences thinking about their mental health. The current crop of such games are just a start, and are understandably quite basic at present, being led by small teams of developers. GenAI could help in two ways here, partly by enabling smaller teams to develop more content, but also by being part of the apps themselves. In particular, GenAI’s ability to create content could prove valuable.
Secondly, in particular cases, digital tools have been used to create ‘avatars’, or virtual personas, for patients to converse with. The early versions of these tools were quite basic, and in some cases literally involve a human on the other end typing out replies to conversations. GenAI has the potential to fill a gap here, allowing such tools to scale out in a way that would previously have been impossible
ADULTHOOD
Ok, so this one is a bit of a cheat. The problem discussed here applies to people of any age. Pressures on outpatient teams mean that in recent years a new service has been developed, “advice and guidance”, that allows GPs to ask questions of the expert team at a hospital rather than referring a patient for an appointment. NHS leadership is keen to expand this service, as it offers a way to avoid unnecessary outpatient appointments. GPs are perhaps less keen, as it puts the ongoing burden of expectation from the patient on them, creates a bottleneck and is ultimately extra work. And it isn’t necessarily quick, it could be weeks of back and forth between GP and hospital before anything happens with the patient.
So how does GenAI help? Well, at present there are over 200,000 monthly advice and guidance requests. In some ways we could model this as a helpdesk, with a user (the GP) consulting with the help team (the hospital) to get a solution to a problem. The question and answer bank is recorded for auditing purposes, much like any helpdesk, so we are slowly over time building up an enormous knowledge base.

It’s now quite common for helpdesks to augment the human team with GenAI via something called ‘Retrieval Augmented Generation’ (RAG). This sounds complicated, but all that happens is that GenAI is used to understand the user’s question, and then query the existing set of Q&As to see if matches can be found. If they can, then a summarised response is either sent to the helpdesk team, or in some cases straight back to the user. We can imagine something similar for advice and guidance, potentially saving time and also picking up on more obscure issues. There’s a huge volume of data being built up, why not use it?
MIDDLE AGE
Menopause has been in the news a lot recently, primarily as women feel that their employers are not sufficiently accommodating to that phase of life. But equally, women don’t feel well supported by the medical profession, with only 12% of women getting a diagnosis from a health professional.
So why is that?
Partly it’s an issue of training, with over half of GPs reporting that they didn’t feel they had enough training relating to the menopause. There’s a particular issue with symptom misattribution, which perhaps isn’t surprising as the menopause can present in numerous different ways often years apart. And underpinning this is a lack of trust, with women feeling they need to take things in to their own hands.

So where does GenAI fit here? Over the coming years it feels certain that GenAI will be used in a diagnostic support role to a growing extent. And the menopause could be a good candidate for this. GenAI excels as taking disparate pieces of information and objectively piecing together a summarisation. In the case of the menopause, with medical records stretching back years and a series of often disconnected symptoms a GP may well not join the dots. But A GenAI-powered tool that had access to GP records probably could, and it could even be integrated with existing apps like the NHS app, to put the information in the hands of citizens.
OLD AGE
As hospital wards come under increasing pressure to clear beds for new patients, the NHS has quietly been testing a new approach in the past few years, Virtual Wards. A patient on a ward goes home, but is not discharged, still being under the care of a hospital team just not in the hospital. They are monitored remotely using a variety of high-tech kit, and after a few weeks if all looks good, they are then actually discharged.
The approach has yielded some positive results but hasn’t been adopted to the extent that the NHS hoped, with less than half the number of virtual ward “beds” in operation and only 4 out of 42 care boards hitting targets by the end of 2023.

So why is this? Partly it’s a question of trust. Clinicians need to feel that patients are actually being adequately cared for, and understandably that’s much easier when they are face-to-face in a ward. It’s also not trivial to decide who ought to go on a virtual ward, requiring additional checks about the patient’s support network and their ability to use technology. And the technology itself can be expensive, requiring a team to help set it up in the patient’s home.
So where does GenAI help? One current problem with Virtual Wards is the hours that they are staffed. In many cases the service is effectively 9-5, and if the patient experiences a problem outside those hours they are told to call 999. That lack of connectivity outside office hours can lead to reluctance on the part of clinicians. But what if there was a halfway option, with a GenAI chatbot deployed to handle first-line patient communication? The chatbot would have a huge advantage over 999 (or 111) in that it would have direct access to a patient’s real-time medical readings, and would be able to guide a patient through a series of questions to determine whether 999 was the most appropriate course of action. By deploying an additional safety net, perhaps consultants would be more willing to move their patients to a virtual ward.
DEATH
Finally, to death, and palliative care.
According to Marie Curie, one in four people die in the UK without access to the palliative care they need, and the demands on palliative care services are predicted to grow by 25% over the next 25 years. The problems are largely due to the pressures discussed right back at the beginning: an ageing population and insufficient funding.
Palliative care is a little different to the other issues we’ve explored in this article, in that the ways GenAI could be applied probably fits numerous aspects of palliative care. There’s a need for greater personalisation, as the material to digest and the decisions that need to be made can be overwhelming. There are mental health issues that could potentially be mitigated through specific digital solutions. Likewise, there are issues accessing information and support 24/7, so chatbot-type solutions might be able to help. Palliative care is an often-overlooked part of healthcare, but the need for novel solutions is no less pressing than the other ages we’ve looked at.
WRAP-UP
So, in conclusion, it’s potentially not so hard to think up ways that GenAI could help mitigate some of the most pressing challenges facing the NHS today. There are four core themes running through the solutions we’ve looked at, and they would be applicable to hundreds more use cases across the healthcare system:
- Information retrieval – the ability to support decisions via surfacing the most pertinent information to users more rapidly
- Content Creation – the ability to scale up content creation at much greater pace and breadth than is currently possible
- Personalisation – tailoring content to the needs of different audiences, be that language, framing or visually
- Interaction – allowing for real-time interactivity with users via chatbots.
If you would like to explore how GenAI might help your organisation, and to learn about the success Agilisys has already had in helping businesses start their GenAI journey, get in touch at info@agilisys.co.uk.





